Malaria

Overview
Malaria is caused by parasites transmitted from person to person by infected female Anopheles mosquitoes—not through casual contact with infected people. There have also been rare cases of malaria transmitted through blood transfusions, organ transplants, shared use of contaminated needles or syringes, and from mother to baby before or during delivery (congenital malaria).
There are four different species of malaria parasites that can be transmitted through the bite of an infected mosquito. Symptoms and severity of infection vary. Symptoms usually appear 7 to 30 days after the infecting mosquito bite, and typically include fever, sweats, headaches, malaise, muscles aches, nausea and vomiting. If malaria exposure is suspected—such as from travel to Africa, Latin America or Asia—a diagnostic test should be performed immediately. Note that antimalarial drugs can delay the appearance of symptoms.
According to the Centers for Disease Control and Prevention (CDC) website, people who have developed protective immunity (mainly adults in high-transmission areas) may be infected but not made ill. Severe malaria occurs more frequently in people with little protective immunity. Complications such as brain disease, severe anemia and kidney failure can develop—and can result in death or life-long neurological impairment. There is no vaccine for malaria, but it is curable if diagnosed and treated promptly.
The CDC website at http://www.cdc.gov/travel/diseases/malaria/index.htm features information on malaria, including advice for travelers to high-risk countries.
Malaria is a parasitic disease caused by a single-celled organism called Plasmodium. It is transmitted through the bite of infected female Anopheles mosquitoes, which are found on every continent of the world. Of the 430 Anopheles mosquito species, only 30-50 transmit malaria. Some Anopheles species prefer to feed on animals, while others feed exclusively on people, including A. gambiae and A. funestus which transmit malaria in Africa.

Anopheles gambiae

Anopheles funestus
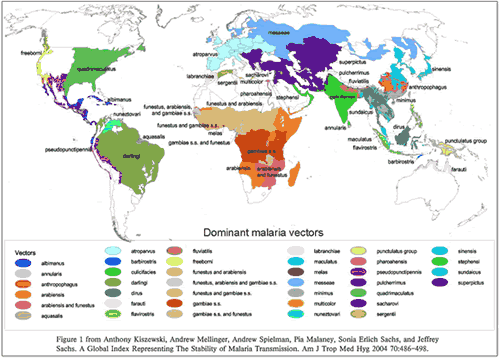
There are four species of Plasmodium: P. falciparum, P. vivax, P. ovale and P. malariae. The illness these parasites cause varies in severity from species to species, but the most dangerous infection is that of P. falciparum—resulting in an estimated 700,000 to 2.7 million deaths annually, mostly in children in Africa. P. falciparum is an extremely rapid and efficient killer; a child infected with this parasite can feel fine in the morning and be dead that night from cerebral malaria. P. ovale and P. vivax have dormant phases where the parasites reside in the liver for months to years, and can cause malaria long after an infective bite.
Plasmodium has a complex life cycle with several intermediate stages, which makes it difficult for the immune system of those infected to fight. Mosquitoes ingest Plasmodium when they bite an infected person. The parasite reproduces in the gut of the mosquito, migrates to the salivary glands and then is delivered into a new host with each bite.
Plasmodium travels through the bloodstream and enters the cells of the liver. It grows and reproduces from several days to several weeks, during which time the infected person experiences no symptoms. At some point, usually between 10 and 15 days after infection, the infected liver cells burst, releasing the parasites into the blood stream where they enter red blood cells. The parasites reproduce rapidly in the red blood cells, causing them to rupture and release millions of parasites into the blood, which then go on to infect additional red blood cells. Each time the red blood cells are reinfected, the host suffers chills, fever, muscle and headaches—typical malaria symptoms resulting from the body’s effort to fight the parasites. Serious complications, including anemia, kidney failure and cerebral malaria, may result from Plasmodium infection—all of which can prove fatal.

Is there malaria in the United States?
Malaria was mostly eradicated from the U.S. and Europe in the 1950s and 60s, largely due to the use of the insecticide DDT. Malaria was reduced in other parts of the world during this time, but once the environmental consequences of the indiscriminate spraying of DDT became apparent, the insecticide was banned in most countries. Additionally, mosquitoes developed insecticide resistance in many areas. These control measures were not implemented in most of Africa. As a result, malaria rates surged in poor countries where other control measures were not available.
If you are traveling to an area where malaria is endemic, you should consult your physician or travel medicine clinic prior to your departure to discuss options for malaria prophylaxis. There are several different drugs available to help prevent malaria, and your physician can advise you on which is the most appropriate for you.
There are a variety of drugs available to treat malaria; unfortunately, they prove cost-prohibitive for the majority of the people who need them in the developing world. Recent initiatives such as the World Health Organization’s Roll Back Malaria Partnership and the President’s Malaria Initiative provide funding for governments in poor countries to purchase these essential drugs. More and more people now have access to these drugs as well as to preventive measures such as insecticide-treated bednets and indoor spraying of insecticides. Time will tell if these initiatives actually reduce the incidence of malaria.
What is the global impact of malaria?
About 40% of the world’s population is at risk for malaria—the majority of which is in developing countries, particularly sub-Saharan Africa. One in five childhood deaths in Africa result from malaria. Non-fatal malaria episodes and constant reinfection cause debilitating chronic illness, leaving people unable to work. Children miss many school days due to illness, and malaria often leads to learning difficulties and reduced cognitive functioning. In countries where the disease is endemic, malaria causes an estimated 1.3% loss of economic growth. Malaria is a disease of the poor, and perhaps more than any other factor, it has limited Africa’s ability to reduce poverty and further development.
I’ve heard that global warming may lead to an increase in malaria worldwide. Is this true?
While predicting global warming trends is difficult, some projections of climate change anticipate a surge in global malaria incidence. This would occur due to shifts in tropical temperatures to more northern and southern latitudes, as well as changing global weather patterns. These models predict changes in a number of vector-borne disease transmission patterns, the impact of which would predominantly be felt in poorer countries.
Is there a vaccine available for malaria?
Efforts are currently underway to develop a vaccine for malaria. The Bill and Melinda Gates Foundation funds a number of vaccine development initiatives. Earlier versions of malaria vaccines have shown poor efficacy in clinical trials. Vaccine development proves challenging, due to the extremely complex nature of the malaria life cycle as well as the parasite’s rapidly-mutating genes.



